Understanding Cancer: Metaplasia
A huge part of modern medicine is cancer, as it’s one of the leading causes of death world wide. I’ve spent the past week and a half learning the basics, so I thought I’d pass it on to anyone who is interested.
The human body is made of trillions of cells but there are different types of cells that we’re comprised of. Each type has a different structure and function as dictated by our DNA, it’s not like there’s just a random cluster of plain cells underneath your skin. Every cell and it’s type plays a role. You can spend a lifetime studying cells alone, they’re fascinating little “worlds”. One of the more interesting aspects to cells is their ability to adapt to harmful stimulus. Cells have efficient regulatory mechanisms to help them adjust, but sometimes a harmful stimulus is just waaaay too much so the cell will actually switch to a type that is better abled to handle the environmental stress. This is called metaplasia.
What do you mean a cell switches types? Well, without giving you an entire course in histology, let’s just look at 2 examples.
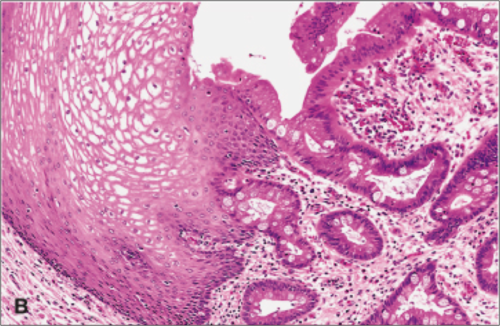
The first is glandular metaplasia, and it can occur in your esophagus at the junction with your stomach. There is a disease that many people suffer from called GERD (Gastroesophageal Reflux Disease). When you eat food it goes through the esophagus and into the stomach, where a muscle-ring called the Lower Esophageal Sphincter closes off to keep the contents of your stomach (food, fluids, and most importantly the acid) from leaking back into your esophagus. In patients with GERD this sphincter is really weak, so the acidic mix of stuff you just ate occasionally squirts back up the tube and damages the parts of the esophagus near the junction. What kind of effect does that acid have on the esophagus? The esophagus is lined with mainly squamous cells. These are simple, run-of-the-mill cells but when they’re constantly getting hit with acid and trying to deal with that kind of damage, they’re going to change into a cell type that’s better able to handle that stress. So they change to glandular cells, like the kind you find in your stomach. These cells secrete mucus that protect them from acid in the stomach so the switch is logical. Basically put, the lower part of the esophagus becomes an extension of your stomach tissue. We call it Barrett’s Esophagus.
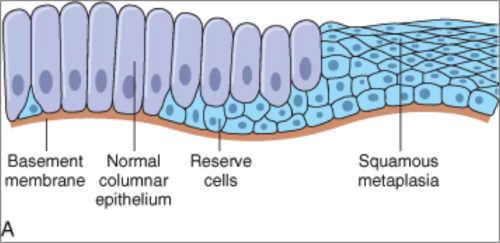
The second example is what happens when people smoke cigarettes for a prolonged period of time: squamous metaplasia. The cigarette smoke is inhaled into the airway and causes chemical damage due to the polycyclic hydrocarbons. This repeated chemical damage forces the glandular cells to switch to squamous cells to better protect themselves. The bad thing about this switch is that these glandular cells in the airways secrete mucus to trap intruders, dust, debris, etc. They also have hairs called cilia that sweep this trapped, mucus coated junk up and out of your airway. This is why smoker’s are vulnerable to constant respiratory infections, their ability to trap and get rid of junk is impaired.
The great news about the metaplasia in both of these cases is that if you remove the irritation, the cells will go back to normal. In the GERD patient we use antacids and look into ways of strengthening the lower esophageal sphincter. In the smoker we… get them to stop smoking. But if it’s reversible what does this have to do with cancer? Well, if the damaging stimulant continues, and these cells keep proliferating and switching, it’s going to increase the risk of developing dysplasia, uncontrolled cell growth. That’s the beginnings of esophagus/lung cancer in these patients.
Credit to white-coat in Tumblr
>>>p./s: that's why, don't smoke!!<<<

2 comments:
hye..! im your new follower..
follow me back ya :))
http://synergistichatidoktormuda.blogspot.com/
Good to have comrade that write sumtin bout medicine too..come to my site jugak okes?
Post a Comment